Top-Down Medicine Is Killing COVID-19 Patients
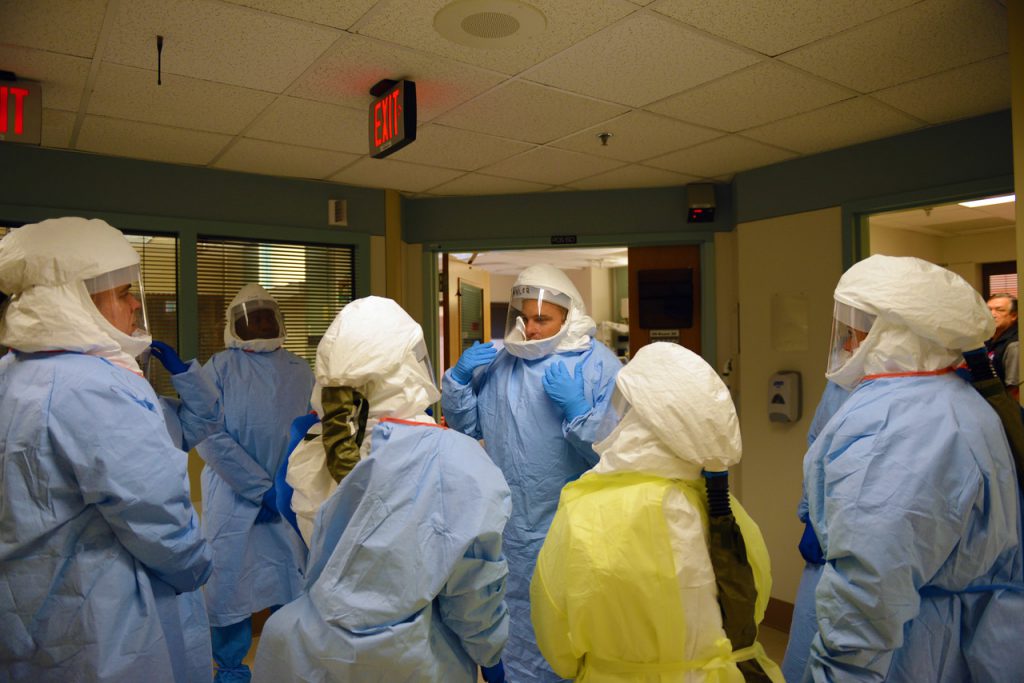
Protocolized medical care is the system in which healthcare professionals use standardized treatment algorithms to treat clinical diagnoses, particularly in critical care areas such as emergency rooms and intensive care units (ICU). Unlike clinical guidelines, which leave room for clinician variations in patient management, protocols are incredibly detailed. Protocols are often computer-based and are specifically designed to decrease clinical errors assuming the complexities of the pathophysiology met with advanced medical technology in patients might exceed a physician’s decision-making capability. Protocols are typically designed by a committee of physicians, nurses, health analysts and hospital administrators to ensure the optimum outcome for their patients.
Treatment protocols ensure that care is evidence-based and up-to-date and this system has no doubt saved lives treating patients with conditions that have anticipated clinical courses.
But we’re seeing that protocol medicine has its limitations. When a novel disease such as COVID-19 makes its way through the population, doctors are using established protocols based on other diseases in the ICU and the results are proving to be disastrous.

While politicians across the country are squabbling over ventilators as the primary equipment needed during the crisis, it is becoming clear that this may not be the best thing for COVID patients—at least the way they are being used now.
From the beginning of the pandemic, the protocol for treating COVID-19 was dangerous for patients. Instead of treating the patient with continuous positive airway pressure (CPAP) machines to get the patient oxygen, medical practitioners were being told to, “let the patient crash and go straight to a ventilator,” as a whistleblower describes in this video:
The DoD COVID-19 Practice Management Guide published March 23 recommends high flow nasal oxygen (HFNC) over BIPAP/noninvasive ventilation (NIV) but if that doesn’t work to intubate early.
Unfortunately, this turned out to be a horribly deadly recommendation.
Typically 40-50 percent of ARDS patients that require ventilator treatment end up dying. For COVID-19 patients, that number jumps to 80 percent. A recent study from Northwell Health COVID-19 Research Consortium showed that upwards of 88 percent of patients who were intubated and put on a ventilator died (compared to just 21 percent of patients who were not put on a ventilator).
Alternative to the Protocol
Last week, a New York City doctor in charge of a COVID ICU, Dr. Cameron Kyle-Sidell, confirmed the general consensus that the novel coronavirus disease was, “unlike anything we had seen.” The standard of care had been to treat patients with severe cases as if they had acute respiratory distress syndrome (ARDS). This would be the logical progression of end-stage severe viral pneumonia that inflicts severe hypoxemic respiratory failure, but he noticed that the treatment algorithm, particularly the ventilator settings for ARDS, was not working on COVID-19 patients.
He reported that the clinical course of the novel coronavirus seemed to appear more like a hematological hypoxemia (abnormally low level of oxygen in the blood) than a respiratory disease, such as ARDS, and that the protocol designated was making it worse for patients by causing ventilator pressure-induced damage to the fragile lung tissue (known as barotrauma).
When he voiced his disagreement with the use of the ARDS protocol, he was met with opposition from hospital administration and ultimately stepped down from his position in the ICU and transferred to the ER where he had more freedom to make his own clinical decisions based on individual patients.
Thankfully, the health establishment is changing its tune. A study in The American Journal of Tropical Medicine and Hygeine states that hypoxemia should not, “not trigger intubation because hypoxemia is often remarkably well tolerated.” And the NIH has updated its COVID-19 treatment guidelines to use noninvasive methods of oxygenation instead of intubation.
“We know that mechanical ventilation is not benign,” said Dr. Eddy Fan, an expert on respiratory treatment at Toronto General Hospital. “One of the most important findings in the last few decades is that medical ventilation can worsen lung injury — so we have to be careful how we use it.”
Politics
Still, making the problem worse is perverse political incentives.
Protocolized medicine is generally thought to protect the patient from financial incentives of bad treatment (eg preventing a physician from prescribing a drug for which he has financial incentive if the drug has not been shown to be effective). But in the case of COVID-19, the financial incentives are for bad treatment.
We’ve reported that physicians are inflating the COVID-19 death statistics, but we’re also seeing government and hospital regulation might make it more likely that COVID-19 patients have bad outcomes.
As Dr. Scott Jensen reported on the Laura Ingram show, “anytime healthcare intersects with dollars it gets awkward. Right now Medicare has determined that if you get a COVID-19 patient admitted to the hospital, you’ll get $13,000. If that patient goes on a ventilator, you’ll get $39,000.” Top-down medicine is incentivizing a failed treatment in the case of COVID-19.
Protocols and evidence-based medicine can be cost effective and life-saving for predictable diseases. As we are learning, however, it can be disastrous for novel diseases like COVID-19. Every hospitalized patient should have been an opportunity to learn more about the disease and, more importantly, the treatment. Top-down medicine that limits the critical thinking and autonomy of physicians to treat individual patients is killing people. Hospital administrators and bureaucrats who refuse to allow treatments that deviate from a prescribed protocol could be partly to blame for the devastating body count left in the wake of COVID-19 pandemic.